- Home
- Your Urethral Reconstruction Journey
Your Urethral Reconstruction Journey
This page gives you a clear overview of your urethral stricture treatment journey.
It is designed to help you understand, anticipate, and prepare for each step with clarity and confidence.

Your stay takes place in a specialized surgical ward, designed for comfort, safety, and close monitoring.
Before Your Hospitalization
Your pathway is carefully prepared in advance. Each step ensures safety and optimal outcomes.
A pre-anesthesia consultation is mandatory. It must take place at least 48 hours before surgery. If you are on treatment, allow 5 days.
Ensure all required investigations are in your file: reports, consultation notes, urethroscopy, urethral imaging, and previous treatment history, etc.
Complete all medical questionnaires, if needed, before admission.
Your signed surgical consent is mandatory. Without it, surgery cannot be performed.
A urine culture (ECBU) is required for urethroplasty at least 7 days before surgery.
Smoking cessation is strongly recommended. Ideally 6–8 weeks before surgery, and continued after surgery. This is essential for healing and surgical success.
Perform hair removal 48 hours before surgery using depilatory cream.
Your Hospital Stay
To help you prepare for your stay, please complete your online admission before your visit. You can also watch the video tutorial for step-by-step guidance.
for step-by-step guidance.
Please come to the clinic with your ID, health insurance card, and any recent paper test results in your possession (blood tests, urine culture, X-rays, CT scan, MRI, etc.).
If you are having surgery the same day, you must come fasting. Do not eat, drink, or smoke for at least 6 hours before arrival.
Also bring loose, comfortable clothes and cotton underwear.

Main Entrance – Groupe Hospitalier Privé Ambroise Paré – Hartmann
48 ter Boulevard Victor Hugo, 92200 Neuilly-sur-Seine, France
Hospitalization Unit
You will be admitted to a specialized surgical ward with dedicated nursing care.
Your stay is organized to ensure comfort, safety, and close postoperative monitoring.
Private, comfortable rooms ensuring rest, privacy, and optimal recovery conditions.

Modern, fully equipped bathrooms designed for comfort and hygiene during your stay.
Your Urethral Stricture Treatment
For Urethroplasty
Your Operation and Hospital Stay
Operation
Urethroplasty procedures typically last 2 to 4 hours and are performed under general anesthesia.
After surgery
After a short stay in the recovery room, you will be taken back to your room. In most cases, you may be discharged within 1 to 4 days after surgery
Dressing and drain
A semi-compressive dressing is usually applied. A drain may be placed, although this is not always necessary. If required, it is usually removed within 1 to 2 days after surgery.
Postoperative pain
Postoperative pain is usually mild. If the pain medication provided is not sufficient, inform the nursing staff or the doctor in charge.
Urinary drainage: urethral catheter and suprapubic catheter
During surgery, urinary drainage is usually provided by:
- a urethral catheter
- a suprapubic catheter (through the abdominal wall)
These catheters allow the bladder to drain properly. The urethral catheter is usually capped and acts as a stent. It is generally removed 5 to 10 days after surgery. Urinary drainage is usually ensured by the suprapubic catheter connected to a leg bag, allowing free drainage of urine and proper healing of the urethral repair.
The suprapubic catheter is usually kept in place for 3 to 5 weeks.
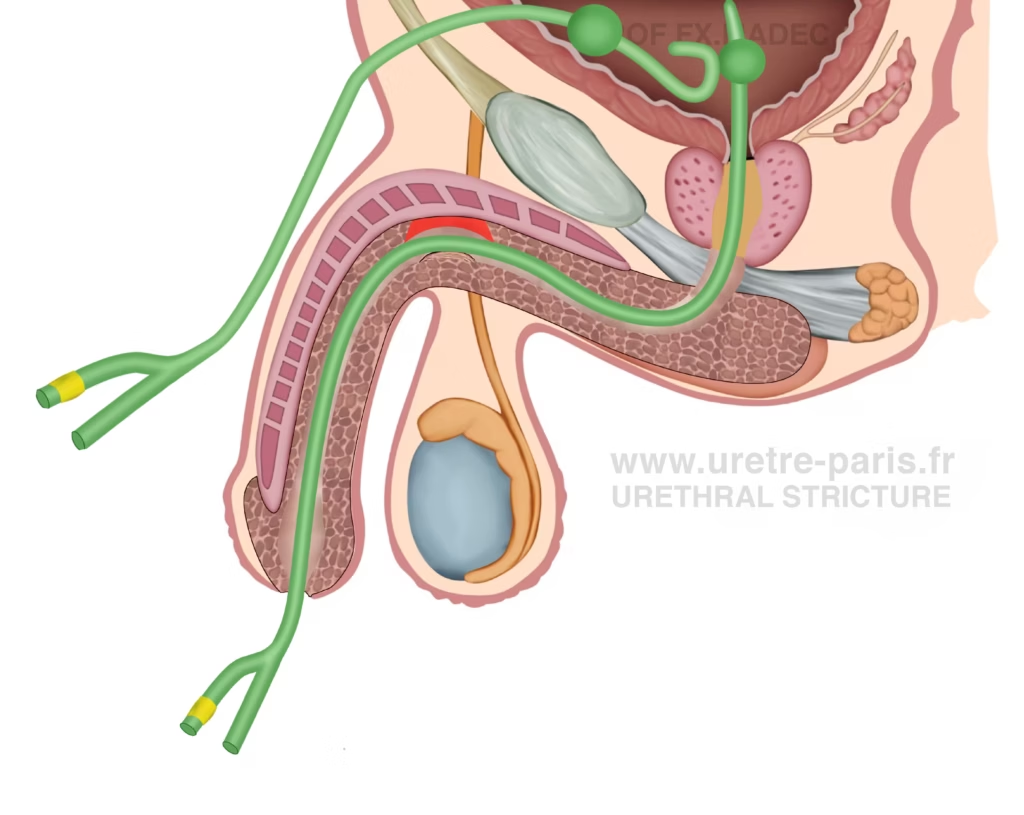
Optimized urinary drainage during the first 10 days after urethroplasty with suprapubic catheter and urethral catheter
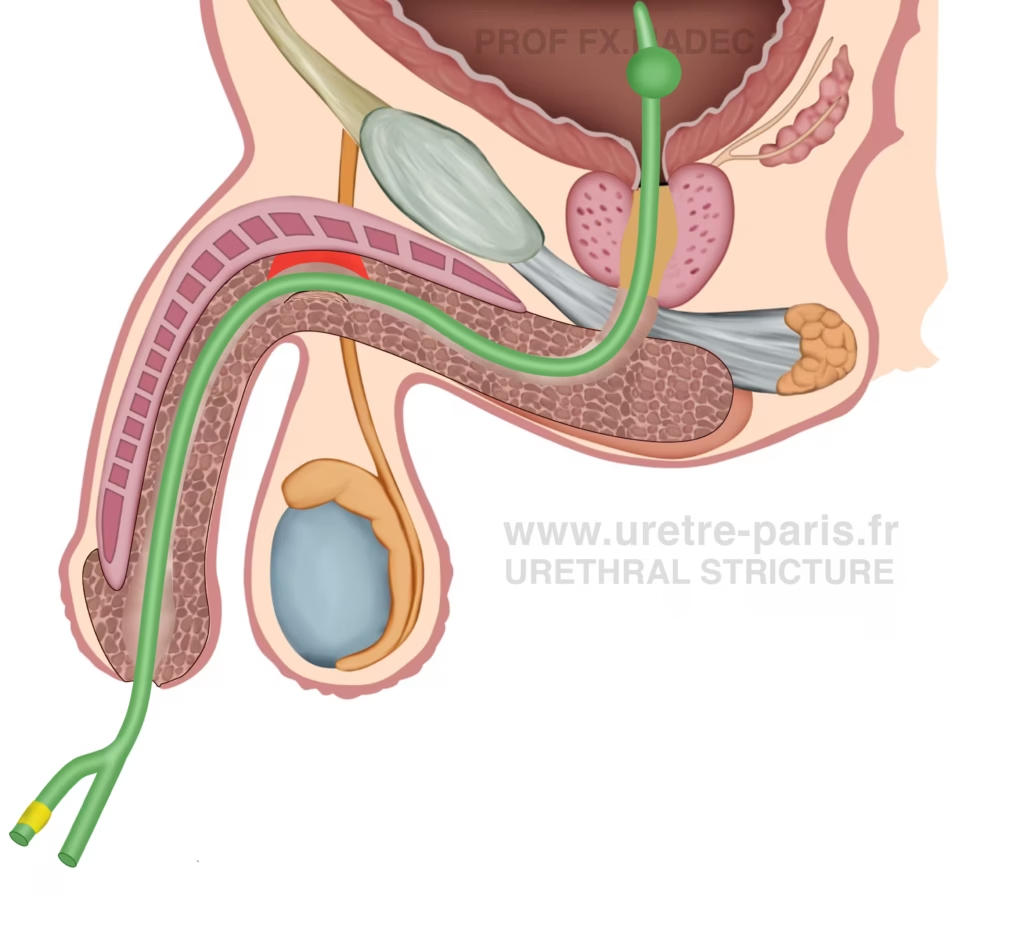
In straightforward cases, a bladder catheter alone may be sufficient during the urethral healing phase after urethroplasty
Mobilization
To promote internal healing, a period of rest may be recommended. In some cases, sitting only on a very soft cushion may be advised. After surgery, ask whether any specific mobility precautions apply in your case.
Food, drink, and mouth care
If a buccal mucosal graft has been harvested, you may usually drink and eat cold soft or blended food from the evening of surgery for 24 to 48 hours. It is best at first to avoid spicy, hard, or crunchy foods, and to chew on the side opposite the graft harvest. If grafts have been taken from both cheeks, blended food may be easier initially. Brush your teeth gently with a soft toothbrush, avoiding the harvest area at first. After that, there are usually no specific dietary restrictions.
Showering
Once the drains have been removed, if any, you may shower after approval from the nursing team. After this type of surgery, two showers per day are generally recommended.
Going Home After Urethroplasty
1 to 4 days after urethroplasty, you are usually allowed to go home.
After urethroplasty, you will usually return home with both a urethral catheter and a suprapubic catheter. Their management requires careful attention, as it is an important part of ensuring optimal healing and a successful surgical outcome. Careful attention must be paid to urine drainage, urine appearance, and the absence of kinking, obstruction, or traction on the catheters. Good hygiene and careful handling are also important throughout this period.
You will receive practical instructions before discharge. Additional information is also provided in your prescriptions and information sheet, and will be explained by the nursing team.
A home healthcare provider may assist with postoperative equipment, dressings, catheter care, and coordination of care at home. A home nurse may also be involved after discharge.
While the catheter is in place, bladder spasms, pelvic discomfort, or an urgent need to urinate may occur. Mild leakage around the catheter can sometimes happen. Specific medication may be prescribed if needed.
Healing, and Recovery of Urination
Healing is monitored closely after surgery. The urethral catheter is usually removed at home by a community nurse, together with any perineal staples, if present.
About 3 to 5 weeks after urethroplasty, the suprapubic catheter is usually clamped and then removed if voiding is satisfactory.
Return to normal activity is gradual. A postoperative sick leave certificate is usually provided for 1 month.
Most sports can usually be resumed after about 3 months. Cycling and straddle sports should be avoided for 12 months. Sexual activity can usually be resumed after about 3 to 6 months.
These timeframes are given as a guide only and must be adapted to your healing, clinical progress, and individual situation.
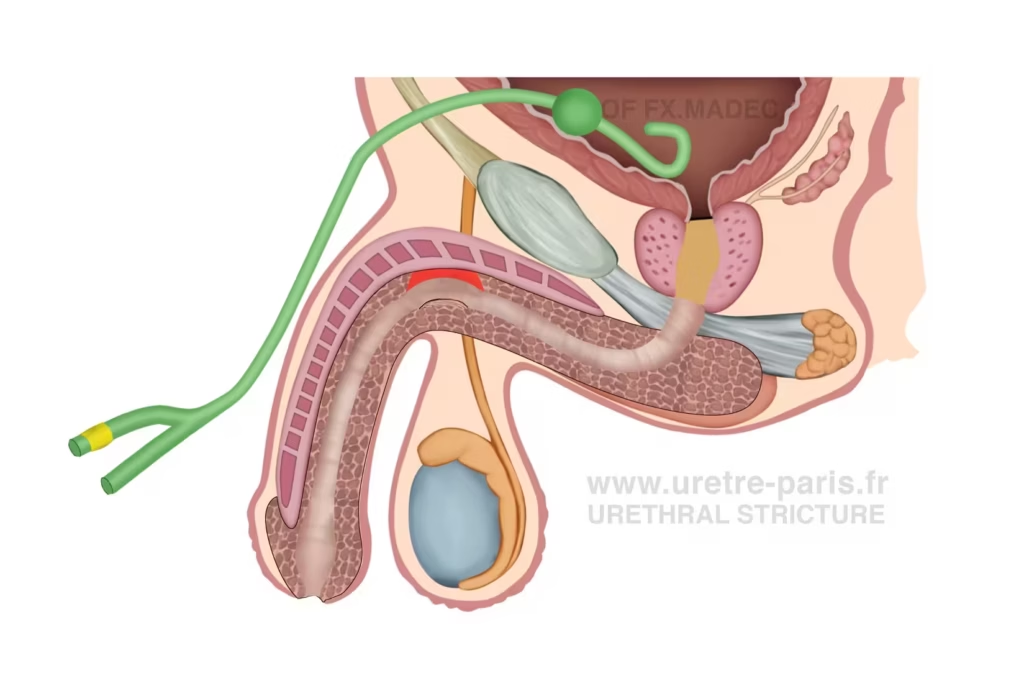
Continued urinary drainage during the final healing phase before catheter removal after urethroplasty
Follow-Up
A follow-up consultation will then be scheduled. Additional investigations may be performed during follow-up, including urethral imaging (VCUG, CT urethrogram, or MRI) and urethroscopy, when needed.
Follow-up includes clinical review, surveillance examinations, and assessment of the functional outcome.
Risks and Potential Complications of Urethroplasty
Because this page focuses on the practical course of treatment and recovery, and although urethroplasty remains the gold standard treatment for urethral stricture disease, a more detailed list of the main potential complications is provided below. This may help you better understand what is common, what is less common, and what may require medical advice.
The following table summarizes the main potential complications and their estimated frequency. Very rare events (<1/250) are not detailed individually.
| Side Effect | Estimated Risk |
|---|---|
| Urinary tract infection requiring antibiotics | 1 in 2 to 1 in 10 |
| Swelling or bruising at the surgical site | 1 in 2 to 1 in 10 |
| Oral discomfort or numbness at the graft site | 1 in 2 to 1 in 10 |
| Post-void dribbling | 1 in 2 to 1 in 10 |
| Stricture recurrence requiring further treatment | 1 in 10 to 1 in 50 |
| Erectile dysfunction potentially requiring treatment | 1 in 10 to 1 in 50 (age/comorbidities dependent) |
| Wound infection requiring antibiotics | 1 in 10 to 1 in 50 |
| Numbness of the posterior scrotum | 1 in 10 to 1 in 50 |
| Fistula (incomplete healing) with urine leakage | 1 in 50 to 1 in 250 |
| Pain during intercourse with reduced ejaculatory force | 1 in 50 to 1 in 250 |
| Persistent oral tightness or lip numbness after graft harvest | 1 in 50 to 1 in 250 |
| Anesthetic or cardiovascular complications (pneumonia, PE, stroke, DVT, MI, death) | 1 in 50 to 1 in 250 (individual risk assessed by the anesthesiologist) |
Healthcare-Associated Infection Risk
As in any hospitalization, there is a risk of healthcare-associated infection, estimated at around 4–6%. This may include infections such as MRSA (Methicillin-resistant Staphylococcus aureus), a bacterium resistant to several antibiotics that can cause skin, wound, or bloodstream infections, and Clostridioides difficile (C. difficile), which can cause intestinal infection, most often after antibiotic use, leading to diarrhea and colitis.
For Urethrostomy or First-Stage Urethroplasty
The overall process is similar to urethroplasty, but usually simpler.
Hospital stay is generally shorter, and recovery is usually faster.
Urinary drainage usually involves only a urethral catheter, which is typically removed 5 to 10 days after surgery.
The rest of the postoperative course is generally similar to that of urethroplasty.
